Synonyms: Submaxillary gland (SMG), Mandibular gland
Definition: Submandibular glands are one of the major salivary glands comprised of mixed serous and mucous acini and located below the lower border of the body of mandible. It is the second largest salivary gland and produces approximately 70% of the saliva.
Location: Submandibular triangle i.e. Level Ib of neck
Parts: The submandibular gland makes a “U” shaped bend around the posterior border of mylohyoid muscle and hence consists of 2 components –
1. Superficial part (larger): below the mylohyoid muscle and fills the digastric triangle
- Lies at the angle of the jaw, wedged between the mandible and the mylohyoid and overlapping the digastric muscle.
- Posteriorly it comes into contact with the parotid gland, separated only by a condensation of its fascial sheath (the stylomandibular ligament).
- Superficially, it is covered by investing layer of deep cervical fascia just beneath the platysma, but it is crossed by the cervical branch of the facial nerve (CN VII) and by the facial vein.
2. Deep part (smaller): above the mylohyoid muscle
- Medially: Hyoglossus and styloglossus muscles
- Laterally: Mylohyoid muscle
- Superiorly: Lingual nerve (CN V)
- Inferiorly: Hypoglossal nerve (CN XII)
Surface marking:
1. Upper margin of gland: Line joining angle of mandible to a point on the middle of the base of the mandible
2. Lower margin of gland: A convex line joining the two ends of upper margin and extending below the level of greater horn of hyoid bone.
Relation to facial artery:
- Grooves the posterior end of gland
- Descends on the lateral surface of gland to reach base of mandible where it comes in close relation to the facial vein
Submandibular duct (Wharton’s duct):
Origin: Deep part of submandibular gland
Length: 5 cm
Triple relation with lingual nerve:
- As the duct exits gland: Inferior to lingual nerve
- As the duct continues distally: Lingual nerve passes below the duct and crosses the duct from lateral to medial (double-crossing)
Relation with sublingual salivary gland:
- The sublingual gland lies immediately lateral to the submandibular duct
Opening: At the sublingual papilla or caruncle by the side of frenulum of tonue in the floor of mouth
Submandibular lymph nodes: Submandibular lymph nodes lie between the gland and the fascial capsule. Occasionally one or more of the lymph nodes may be embedded deep within the salivary gland. The nodes are small, usually measuring approximately 1 centimeter in a healthy adult.
Arterial supply: Branches of facial and lingual arteries
Venous drainage: Common facial vein and lingual vein
Lymphatic drainage: Submandibular lymph nodes
Innervation: Innervated by parasympathetic secretomotor fibers from the facial nerve, which run in the chorda tympani and in the lingual nerve and synapse in the submandibular ganglion. It also have sympathetic innervation from superior cervical ganglion.
Clinical Correlation:
1. Bidigital or Bimanual palpation of the gland:
- Index finger of a gloved hand is passed below the tongue in the floor of mouth (for deep part or lobe of gland)
- Index finger of another hand is placed antero-medial to the angle of mouth (for superficial part or lobe of gland)
- It is helpful in differentiating the gland from the enlarged submandibular lymph node, which is palpable only antero-medial to the angle of mouth and not intra-orally.
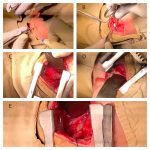
2. Excision of submandibular gland:
The excision of gland may be indicated for chronic sialadenitis, submandibular gland calculi and suspected submandibular neoplasm. This operation is carried out through a skin crease incision 5 cm below the angle of the jaw. This is done in order to preserve the mandibular branch of facial nerve (CN VII) which passes behind the angle of jaw rather less than 1 inch (2.5 cm) from it.
3. Block dissection of neck: The presence of small lymph nodes in close proximity to the gland or within the substance of the gland makes removal of the gland an imperative part of block dissection of the neck.
4. Sialolithiasis: Calculi are most common in the sabmandibular gland due to following reasons –
- Viscid sero-mucinous secretion
- Long and curved duct
- Calcium salts in secretion
- Antigravity drainage
- The duct is crossed by lingual nerve


I love your diagrams