History
23yrs/F non-diabetic, non-hypertensive, non-smoker, non-alcoholic primigravida was admitted to Obstetric ward on with the chief complaints of:
- Cessation of menstruation X 9 months
- Decreased fetal movement X 6 hours
| LMP | 2072/04/12 |
| EDD | 2073/01/19 |
| GA | 41 WOG |
Examination
| General condition | Fair |
| Pallor | Absent |
| Icterus | Absent |
| Edema | B/L pitting – pedal |
| BP | 120/90 mmHg |
| Pulse | 90/min |
| Per Abdomen | |
| Uterus | Term size |
| Lie | Longitudinal |
| Presentation | Cephalic |
| Head | 5/5 palpable |
| FHS | +; 140/min |
| Per Vaginal Examination | |
| Cervical os | 3 cm |
| Effacement | 50% |
| Fetal head station | -3 |
| Membrane | Present |
| Show | Present |
Provisional Diagnosis: Primigravida at 41 WOG in Latent Phase of Labor
- All ANC investigations were normal.
- ARM was done, which showed moderately meconium stained liquor.
- Patient was shifted to OT for Em. LSCS for fetal distress and Em. LSCS was done.
| OT findings | |
| LUS | Well formed |
| Liquor | Moderately meconium stained; adequate |
| Presentation | Cephalic |
| Placenta | Fundo-posterior |
| Tubes & ovaries | B/L normal |
| Outcome |
| Single, Alive, Term, Male baby with birth weight of 3.2 Kg at 2:16 PM on 2073/1/26 with cord around neck (once; loose) with APGAR Score 8/10 and 9/10 |
| Post-op BP | 200/110 mmHg |
| Total Blood Loss | 400 ml |
Postoperative Period
- On the day of operation – patient developed GTCS lasting ~30 seconds with BP: 200/120 mmHg; Pulse: 120/min and SpO2: 83%
- Management:
- Patient was placed in left lateral position and Oxygen was given
- Inj. MgSO4 loading dose stat
- Inj. Lorazepam 4 mg iv stat
- Inj. Lasix 20 mg iv stat
- Patient was shifted to ICU
- Patient was kept NPO and IV fluids were given
- Foley’s catheter was insitu
- PIH investigations were sent urgently
- Diagnosed with postpartum eclampsia
Results of PIH investigations
- Uric acid – 5.4 mg/dl (raised)
- LDH – 847
- Urine albumin – Nil
- 24 hour urine protein – 324 mg/24 hour (raised)
- Hb, Platelets, BT/CT, RFT, LFT and Urine R/E were within normal limits
In ICU
- Patient received maintenance dose of MgSO4 every 4 hourly for 24 hours following the seizure (5 doses) as per Pritchard regimen
- Blood pressure, Pulse rate, Respiratory rate, Urine output and Patellar reflex were monitored hourly
- BP range: 120-150/70-90 mmHg
- Pulse rate: 82-120/min
- Respiratory rate: 15-22/min
- Urine output: 50-300 ml/hr
- Patellar reflex: Present
- Patient received Tab. Nifedipine 10 mg PO stat at 6 PM
In Subsequent Postoperative Days
- No further episodes of seizure
- GCS was 15/15; BP ranged from 130-150/70-80 mmHg
- Other vital signs were also stable
- Chest, CVS and CNS examination were normal
- Urine output was maintained
- Involution of uterus was normal
- Patient was transferred out of ICU after 2 days
Discharge
- Patient was discharged on 5th postoperative day
- BP at the time of discharge: 100-130/70-90 mmHg
- Patient was discharged on:
- Antihypertensive: Tab. Depin Retard 20 mg PO BD for 7 days
- Oral antibiotics
- Analgesic and H2 blocker
- Iron and Calcium
- Patient was advised to follow up after 1 week/SOS
Review of Pre-eclampsia and Eclampsia
- Hypertensive Disorders in Pregnancy
- Pritchard Regimen for Magnesium Sulfate
- Approach to hypertensive disorder in pregnancy

Lets revisit the management of Eclampsia in detaile here:
Screening for PIH
- Roll-over test: Rise of DBP by 20 mmHg or more after turning from left lateral to dorsal position
- Hand-grip test: Rise of DBP by 20 mmHg or more at 28-32 WOG after compressing inflated sphygmomanometer for 3 minutes
- Forearm venous tone: Increased tone atleast 6 weeks before diagnosis of PIH (requires sophisticated equipment)
- Urine assays: Micro-albuminuria, lower 24 hr urinary Ca++ excretion, reduced kallikrein/creatinine ratio, increased PG metabolites
- Blood tests: Increased plasma urate, reduced platelet count, reduced anti-thrombin III activity 1
6 Stages of Management of Eclampsia
- Making sure the airways are clear and the woman can breathe
- Controlling the fits
- Controlling the Blood Pressure
- General care and monitoring, including controlling fluid balance
- Delivering the baby
- Monitoring carefully to prevent further fits and identify complications 2
Making sure the woman can breathe
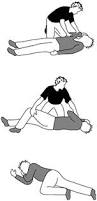
Left lateral position
Oxygen (if available)
- Continue for 5 minutes after each fits
- Or longer if cyanosis persists
Aspirate mouth and throat after convulsion
Stay with woman and ensure her airway is clear
Controlling the fits
Anticonvulsant of choice:
- Magnesium sulfate
- Diazepam (if Magnesium sulfate unavailable)
Diazepam:
Diazepam can cross the placenta and cause neonatal respiratory depression, difficulties with feeding and in maintaining body temperature. Do not give more than 100mg of diazepam in 24 hours.
- Loading dose:
- 10mg IV slowly over 2 minutes
- If convulsions recur: repeat the loading dose
- Maintenance dose:
- 40mg in 500ml IV RL/NS
- Titrate to sedation but arousable
- Complication:
- Maternal depression may occur when >30mg in 1 hour
- Can be given PR:
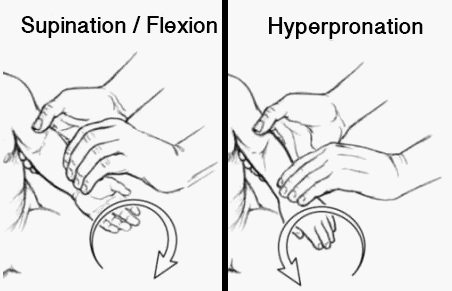
- Give 20mg in a 10ml syringe → Remove needle → Lubricate barrel → Insert syringe into rectum to ½ the length → Discharge the contents and leave syringe in place → Hold buttocks together for 10 mins to prevent expulsion of contents
Collaborative trial for Eclampsia
- International multi-center Eclampsia trial in 1680 eclamptics
- Magnesium sulfate was found to be superior than Diazepam and Phenytoin
- Fewer recurrent convulsion: 5.7%
- 27.9% for Diazepam
- 17.1% for Phenytoin
- Fewer maternal death: 2.6%
- 5.1% for Diazepam
- 5.2% for Phenytoin 3
Magpie trial
- Prospective RCT conducted at 175 hospitals in 33 countries
- Originally included 8804 women with pre-eclampsia randomized to Magnesium sulfate or placebo
- Concluded the beneficial role of Magnesium sulfate:
- 58% lower relative risk of eclampsia
- 45% lower relative risk of maternal mortality
- Significantly lower risk of placental abruption (2% vs 3.2% with placebo)
Controlling the Blood Pressure
- Indication of antihypertensives: DBP ≥110 mmHg
- Aim: DBP 90-100 mmHg (to prevent cerebral hemorrhage)
- Drug of choice: Hydralazine
- 5 mg IV slowly every 5 min until BP ↓
- Repeat hourly as needed OR give 12.5 mg IM 2 hrly as needed
- Alternative: Labetalol 10 mg IV
- Dose can be doubled every 10 min upto 80 mg (10→20→40→80) until BP ↓
General Care
- Minimum external stimulus (noise, bright lights, handling)
- Never left alone
- Anesthetic instruments, suction apparatus & O2 equipment – at bedside
- Turn the patient 2 hrly – to prevent hypostatic pneumonia
- Mouth care (No oral fluids given)
- Urinary catheterization and monitoring of urinary output
Monitoring
- Restlessness or twitching – may precede another fit
- Color for cyanosis – indicates need for oxygen
- Temperature 4 hrly – hyperpyrexia may occur
- Pulse and respiration hourly or more often
- Blood Pressure atleast hourly
- Fetal heart rate hourly
- Signs of labor
- Fluid balance is recorded accurately
Delivering the baby
- As soon as condition stabilized:
- Within 24 hours from symptom onset in severe pre-eclampsia
- Within 12 hours from convulsion in eclampsia
- Indication of CS:
- Unfavorable cervix
- FHR abnormalities (<100 bpm or >180 bpm)
- If Vaginal delivery is not anticipated within 12 hrs of eclampsia and 24 hrs of severe pre-eclampsia
Care after the delivery
- Fits can:
- Occur for the 1st time after delivery, within the 1st 48 hours
- Recur after delivery
- Continue:
- Careful observation for ≥ 48 hours
- Anticonvulsant for 24 hours after delivery or last convulsion (that occur last)
- Monitoring urinary output (tendency to retain fluid and increase BP)
- Shift to main ward (with 4 hrly BP checks) if after 48 hours:
- No fits
- Good urinary output
- DBP <110 mmHg
Counselling
- Greater risk of having underlying medical condition
- 20-40% develop chronic hypertension – close f/u necessary
- Reccurence:
- 65% if pre-eclampsia develops in midtrimester
- 20% if pre-eclampsia develops at term
- 3% reccurence of HELLP
- 1-2% reccurence for eclampsia 4
Calcium supplementation to prevent PIH
- Randomised trials comparing at least 1 g of calcium daily during pregnancy with placebo
- Twelve studies (15,528 women) were included
- 30% reduction in the risk of gestational hypertension
- 20% reduction in maternal mortality and morbidity
- Low calcium intake may cause high BP by stimulating either:
- Parathyroid hormone or
- Renin release, thereby increasing intracellular calcium in vascular smooth muscle and leading to vasoconstriction

He is the section editor of Orthopedics in Epomedicine. He searches for and share simpler ways to make complicated medical topics simple. He also loves writing poetry, listening and playing music. He is currently pursuing Fellowship in Hip, Pelvi-acetabulum and Arthroplasty at B&B Hospital.