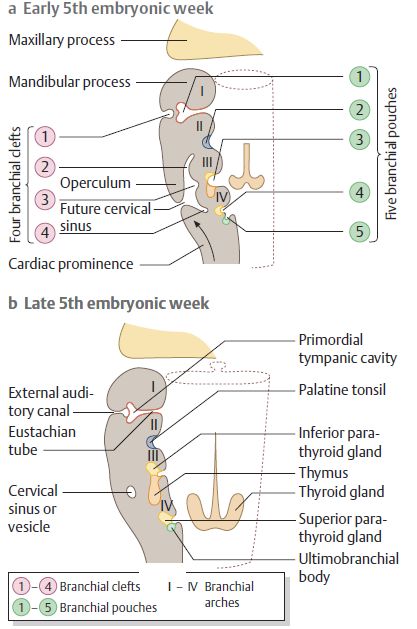
Epineurium of sciatic nerve (like all other nerves) is continuous with the duramater withing the spinal canal which is firmly attached to the foramen magnum above and the filum terminale below. In the elastic neuromeningeal pathway, tension applied at one point will spread through out the length of spine until it is constant all over. Flexion of the trunk would lengthen the spinal canal stretching the dura and extension would shorten the same resulting in relaxation.
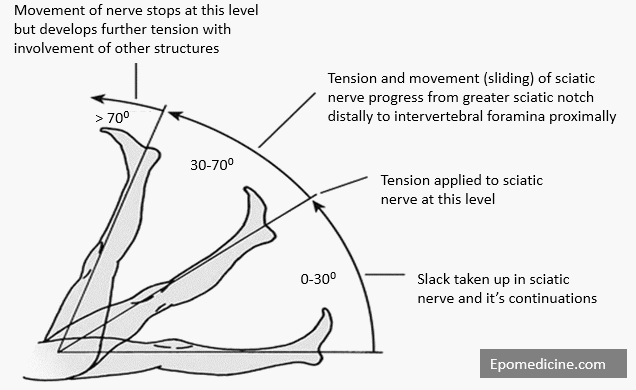
First 30 degrees of SLR serves to take up the slack or crimp in the sciatic nerve and its continuations. Between 30 and 70 degrees, the spinal nerves, their dural sleeves and roots of the L4, L5, S1, and S2 segments (S3 root doesn’t reach the lower limb) are stretched with an excursion of 2-6 mm. Tension and movement first develop at the sciatic notch, then over the ala of sacrum, then as the nerve crosses over the pedicle, and finally at intervertebral foramen. The nerve roots also move laterally toward the bone and therefore move into a posterolateral herniation and potentially away from a central herniation. Therefore a midline herniation may not cause sciatica during straight leg raising and the test will be negative. Movement of the nerve past neighouring structres stop altogether as the leg is raised past 70 degrees. After 70 degrees, although these structures undergo further tension, other structures also become involved.
In short, following events occur in sciative nerve during SLR test:
0-30 degrees – Tone the slack
30-70 degrees – Sliding and stretching
70-90 degrees – Only stretching
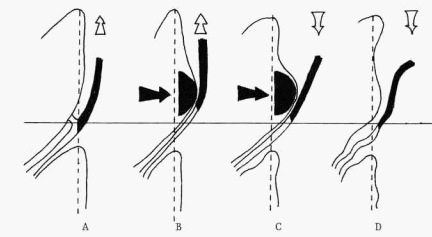
C (disc protrusion) and D (normal) during relaxation
Here, it is imperative to mention Breig’s tissue borrowing phenomenon. The tension produced in a lumbosacral nerve root results in displacement of the neighboring dura, nerve roots, and lumbosacral plexus toward the site of tension. In effect, a borrowing of the resting slack in neighboring meningeal tissues occurs as neural structures are pulled toward the site of increased tension. This stretching and displacement of the nerve roots plexi reduces the available slack and potential mobility of the peripheral nerves.
In short, in cases of prolapsed disc, some of the normal available slack is taken with increase in resting nerve root tension, in effect, priming it for the subsequent test.
The SLR test will cause traction on the sciatic nerve, lumbosacral nerve roots, and duramater. Adhesions within these area may be caused by herniation of the intervertebral disc or to extradural or meningeal irritation.
SLR test in uninvolved leg (crossed SLR or ‘well leg’ test) pulls the nerve root and dura distally and medially, but raises the pressure on the nerve complex by less than half of the standard SLR test in involved leg. This means, if the corssed SLR is positive, the resting tension of these tissues must be higher to cause pain with lesser stretch than the standard SLR and hence, it is considered more reliable.
While the SLR test can be positive in varied conditions, its value of diagnosis for confirmation of nerve root as the source of pain can be improved lowering it a few degrees (about 10 degrees) until pain improves. From this point, the neuromeningeal structures can be further stretched by 3 maneuvers which are called as sensitizers:
- Passive dorsiflexion of the foot (Braggard’s test)
- Applying firm pressure to lateral popliteal nerve behind the lateral tibial condyle, to tighten it like a bowstring (Bowstring test)
- Passiver cervical flexion (Soto-Hall test)
References:
- Dutton’s Orthopedic Examination, Evaluation and Intervention – 3rd Ed.
- The Straight-Leg-Raising Test: A Review by LAWRENCE M. URBAN, BA, DPT
- Illustrated Orthopedic Physical Assessment – E-Book by By Ronald C. Evans
- Managing Sports Injuries by Christopher M. Norris – 4th Ed.