In medical school, coagulation cascade might be a pain to learn and teach as well. Plenty of roman numerals with arrows going here and there – is this the reason you hate coagulation cascade? I will pretty much try to simplify the whole thing with essential clinical correlation here. I know many of you are tempted to mug up the cascade without understanding it and print it in examination. But that is not going to help and I recommend you to spend a few minutes learning the coagulation cascade and not just reading it.
Coagulation factors – Mnemonic
During medical school, I read this mnemonic in a book and it still comes handy:
First Person Told Cancer Leads Sickness, Another Chap Said Protein High Fat
- Factor I: Fibrinogen (First)
- Factor II: Prothrombin (Person)
- Factor III: Tissue thromboplastin or Tissue factor (Told)
- Factor IV: Calcium (Cancer)
- Factor V: Labile factor (Leads), Proaccelerin
- Factor VI: Accelerin (Remember: has been eliminated as it plays no role in blood coagulation)
- Factor VII: Stable factor (Sickness), Proconvertin
- Factor VIII: Anti-hemophilic factor A (Another)
- Factor IX: Christmas factor (Chap), Anti-hemophilic factor B
- Factor X: Stuart power factor (Said), Autoprothrombin III
- Factor XI: Plasma Thromboplastin Antecedent or PTA (Protein)
- Factor XII: Hageman factor (High), Glass or contact factor
- Factor XIII: Fibrin stabilizing factor or Fibrinase (Fat)
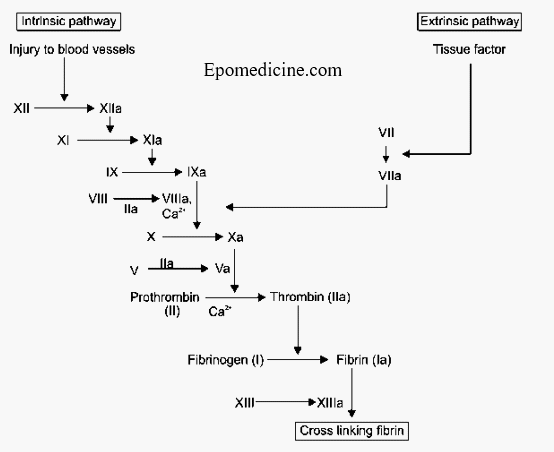
Coagulation Cascade – Simplified
For a complex and detailed cascade, refer to a textbook.
1. Aim of coagulation cascade is to lay down fibrin, hence the final step involves:
- Factor I: Fibrinogen which is converted to Fibrin
- Factor XIII: Fibrin stabilizing factor which cross-links the Fibrin
2. Coagulation cascade is activated by 2 pathways, the extrinsic and intrinsic which culminates into a common pathway. The factors involved in common pathway can be remembered by a mnemonic: 1 X 2 X 5 = 10.
- Factor II (prothrombin): when activated to thrombin, activates factor I and XIII
- Factor V (labile factor): when activated, activates factor II
- Factor X (Stuart power factor): activated by both intrinsic and extrinsic pathway; when activated activates factor II
3. Extrinsic pathway (Tissue factor pathway):
Mnemonic: Tissue factor is factor 3 and 3 + 7 = 10 (Common pathway). Hence, factors involved in Extrinsic pathway are factor III and factor VII.
4. Intrinsic pathway (Injury pathway):
Mnemonic: Factors 12 to 8 are involved in intrinsic pathway, excluding factor 10 which is a part of common pathway. Hence, factors involved in Intrinsic pathway are: factor XII, factor XI, factor IX and factor VIII.
Facts to remember about clotting cascade
1. All clotting factors are proteins and synthesized in liver except:
- factor IV: calcium
- factor VIII carrier protein: vWF (vonWillebrond factor)
2. Remember a small loop of positive feedback in common pathway:
- Activated factor V (Va) activates factor II (IIa or thrombin)
- Activated factor II (IIa or thrombin) activates factor V.
3. Factors II, VII, IX and X require Calcium (factor IV) and Phospholipid (PL) for activation. These are vitamin K dependent coagulation factors and affected most by liver disease and warfarin. Extrinsic pathway is affected and hence, PT/INR is elevated. Normal PT is 12-16 seconds. Prothrombin Time (PT) and International Normalized Ratio (INR) are same thing. INR is ratio of PT of patient with that of control. If PT of patient is same as that of control, then INR is 1. Deficiency of vitamin K is also responsible for Hemorrhagic disease of newborn. The release of delta granule from platelets result in release of calcium required for coagulation cascade during hemostasis.
4. When the extrinsic pathway progresses into common pathway, factor Xa interacts with TFPI (Tissue factor pathway inhibitor) and turns off the extrinsic pathway by inhibiting VIIa and Xa. However, factor Xa also activates factor II (prothromin) to thrombin which in-turn activates intrinsic pathway (factor XI and factor IX).

5. Antithrombin III inhibits factor IIa (thrombin) and factor X. Anti-thrombin III mechanism also belongs to heparin. Intrinsic pathway is affected and hence, aPTT (activated Partial Thromboplastin Time) is elevated. Normal aPTT is 26-34 seconds.
6. Protein C, S and thrombomodulin inactivates factor V and VIII through activated Protein C. These are also Vitamin K dependent and warfarin (vitamin K inhibitor) given may initially have paradoxical pro-coagulant effect due to inhibition of Protein C and S. Hence, to prevent this complication, it is co-adminsitered with heparin for few initial days. Deficiency of Protein C leads to thrombophilia. Thrombomodulin is produced by all endothelial cells except those in the cerebral microcirculation. Thrombin-thrombomodulin complex is an anticoagulant.
7. Tissue plasminogen activator (tPA) like streptokinase converts plasminogen to plasmin. Plasmin degrades fibrin and hence, tPA are used as thrombolytics or fibrinolytics.
8. Factor XII is the only protein in the coagulation cascade whose deficiency does not cause bleeding but rather results in a prothrombotic state.
9. Hemophilia results from deficiency of factor VIII or IX. Though the extrinsic pathway is normal, bleeding manifestation is due to:
- Inadequate fibrinogenesis
- Inappropriate fibrinolysis – very high levels of thrombin are required to activate TAFI (thrombin activatable fibrinolysis inhibitor) that augments fibrin deposition by inhibiting fibrinolysis.
10. Factor V leiden leads to thrombophilia rather than hemorrhagic disorder. This is because, factor V leiden are mutated factor V that possess normal factor V activity but resists inactivation by activated protein C. It is the most common inherited cause of hypercoagulability in which normal arginine is replaced by glutamine at position 506 making it resistant to degradation by protein C.
11. Haemophilia A, B (Haem-A, B) and von Willebrand disease (vWD) are the most common inherited coagulation disorders, whereas congenital deficiencies of FI, FII, FV, FVII, FX, FXI, FXII or FXIII occur rarely. Factor XIII may commonly present at birth with bleeding umbilical stump, cephalhematoma and intracranial hemorrhage.
12. Thrombin time (TT) is used for testing the conversion of fibrinogen into fibrin and depends on adequate fibrinogen level.
13. Fibrin Degradation Products (FDP) is used to assess fibrinolytic activity and are increased in Disseminated Intravascular Coagulation (DIC).
14. Bleeding time (BT) is an assay to test platelet function. Normal Bleeding Time is 2-9 minutes. It is prolonged in quantitative or qualitative platelet disorders.
15. Factor XIIa (Hageman’s factor) also initiates kinin system by converting pre-kallikrein to kallikrein which inturn converts kininogen to kinin (bradykinin). Activated factor XII can cause activation of kinin system, clotting system, fibrinolytic system and the complement system.
16. Fresh Frozen Plasma (FFP) contains all factors of the soluble coagulation system and is indicated in bleeding patients and patients with multiple factor deficiencies.
17. Cryoprecipitate is a concentrated fraction of FFP which is rich in factor I (fibrinogen), factor VIII, factor XIII and vWF and hence is indicated in hypofibrinogenemia, vonWillebrond disease and hemophilia A. It only contains 40-50% coagulation factors found in FFP but is concentrated and has less volume.
18. After an injury, following transient vasocinstriction mediated by endothelin, there is release of tissue factor from the injured cells activating the factor VII (extrinsic pathway) and exposure to subendothelial collagen causing activating of factor XII (intrinsic pathway).
19. Tenase complex: Activating complex of factor X (ten) –
- Intrinsic tenase complex: IXa + VIIIa + Calcium
- Extrinisc tenase complex: Tissue factor + VII + Calcium

He is the section editor of Orthopedics in Epomedicine. He searches for and share simpler ways to make complicated medical topics simple. He also loves writing poetry, listening and playing music. He is currently pursuing Fellowship in Hip, Pelvi-acetabulum and Arthroplasty at B&B Hospital.
Awesome work
Thank you very much.
WHY IS D DIMER VERY HIGH IN ACUTE PROMYELOCYTIC LEUKAEMIA?
Because in PML there might be overactivation of coagulation because of exposure to tissue factor in the granules contained in the abnormal promyelocytes. The presence of clots causes massive fibrinolysis, resulting in high FDP and a bleeding diathesis.
Been following epomedicine for a long time.
Correct and condensed info
Great work Dr Sulabh🙌
I found you through a recommendation from my lecturer Mr Simon and I am so glad! First year of medicine, so I must admit some of the content got slightly overwhelming. but I appreciate your straight forwardness. Looking forward to digesting your entire website hahaha~ Thank you!
Excellent work putting together very condensed and useful information. The “cream.”
Very clear, easy to understand.
NYC VIEW DR
I h8 9 11 because it makes New York Partial => factors 8, 9 and 11 determine the “Partial” thromboplastin time
Where did the planes go on 9 11 ? IN Towers => factors 9 and 11 which determine the “Partial” thromboplastin time, are part of the INTrinsic pathway
Added bonus for “h8 9 11” :
Haemophilia A = factor VIII mutation
Haemophilia B = factor IX mutation
Haemophilia C = factor XI mutation
Very concise information. Thank you for your effort.