A Single/ Term Male Baby weighing 3.0 kg was delivered via emergency LSCS for fetal distress who was prenatally diagnosed to have congenital diaphragmatic hernia in utero. He was born with Apgar score 4/10, 6/10, was immediately intubated and transferred to NICU. After stabilization, he was kept under the ventilator and planned for surgery by the Pediatric surgery team.
Chest Xray – showed bilateral severe pulmonary hypoplasia with intestinal content in the left chest with displacement of the mediastinum to the right.
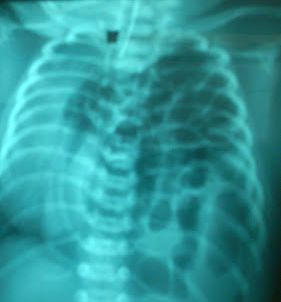
Almost entire bowel loops were in the chest.
Initial Stabilization until intubation can be done with:
1. Oxygen by blow-by and insert 10 F Orogastric tube. Remove air manually by aspiration.
2. Attach the OG tube to an intermittent suction device set at 40 mmHg pressure or do frequent manual aspirations.
3. Get a Chest Xray and be sure gastric tube is in place. Locate the stomach.
4. Make sure of adequate oxygenation to prevent PPHN.
5. Evlauate for PPHN with preductal and post ductal saturation measurements.
6. Maintain adequate hydration and if needed – Inotropic support.
7. Watch closely for Pneumothorax.
8. Keep the infant calm with analgesia.
In such scenario:
1. Bag and Mask Ventilation is contraindicated as it inflates the gut, further compromising the lung functions.
2. Intubation and Bagging should be done and NG tube should be inserted. Intuabtion is preferred with a cuffed ET tube.

MD Pediatrics and Fellowship Neonatology, he chooses to stay anonymous. He often writes his views online as well as share few important topics for medical students, doctors and specially parents. He does research in pediatrics.