GASTROESOPHAGEAL JUNCTION (CARDIA)
It is the junction between esophagus and cardia of stomach
Histologically: Mucosal transition from squamous to columnar epithelium
Functionally: High pressure zone (Lower esophageal sphincter or LES) – Normally, LES is intraperitoneal, >2 cm long, and has a resting pressure >6 mmHg; not an anatomical sphincter but a physiologic sphincter, the mechanism of which is unclear.
- Mucosal folds at this level acts as valve
- Acute angle of entry of esophagus into stomach produces valve-like effect
- Circular muscles of lower esophagus is a physiological sphincter
- Arrangement of muscle fibers around cardia acts either as sphincter or maintains acute angle of entry of esophagus into stomach
- Right crus of diaphragm acts as a “pinch-cock” to the lower esophagus as it pierces the diaphragm
- Positive intra-abdominal pressure compresses the walls of the short segment of intra-abdominal esophagus
GASTRODUODENAL JUNCTION
It is the junction between pylorus of stomach and duodenum
Histologically: Mucosal transition from gastric to intestinal epithelium (striated columnar cells with interposed goblet cells)
Functionally: Smooth muscle valve i.e. Pyloric sphincter surrounding pyloric canal
Externally: Marked by the crossing of constant vein of Mayo (also known as prepyloric vein – a tribuatry of the right gastric vein that passes anterior to the pylorus at its junction with the duodenum).
DIVISIONS OF STOMACH
Fundus (Proximal portion)
- Undergoes receptive relaxation (vagovagal reflex): As food enters the pharynx and esophagus, vagal stimulation causes relaxation of fundus, limiting rise in intragastric pressure as the food is stored; it is abolished by vagotomy
- Site of autonomic pacemaker (interstitial cells of Cajal): Initiates intragastric motor activity
- Function: Storage of food
Gastrointestinal Stromal Tumor (GIST) originates in pacemaker of stomach (interstitial cells of Cajal).
Corpus or Body (Middle portion)
- Cells: Majority of parietal cells (acid producing), Chief cells (pepsinogen producing) and Enterochromaffin like (ECL) cells
- Function: Hydrochloric acid (HCl) secretion, Storage, Peristaltic grinding against pylorus
Antrum (Distal portion)
- Cells: “G” cells (gastrin producing)
- Junction of the body with antrum: marked by distinct notch on the lesser curvature known as incisura angularis (junction between the vertical and horizontal parts on the lesser curvature side of ‘J’-shaped stomach)
- Surgeon performing an antrectomy for ulcer disease must be certain to extend the resection to the proximal duodenum, since retained antrum in this now isolated, non–acid containing segment will hypersecrete gastrin causing recurrent ulcers in the remaining proximal stomach or at the anastomosis to small bowel (marginal ulcer).
Note: Mucus secreting goblet cells are found throughout the stomach
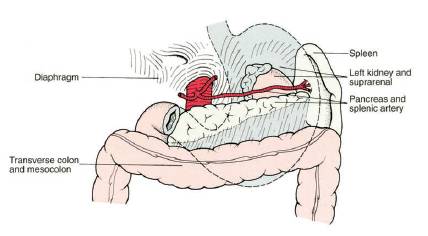
RELATIONS OF STOMACH
1. Superiorly: Diaphragm
2. Inferiorly: Greater omentum
3. Laterally: Spleen and Liver
4. Anteriorly: Diaphragm and Left lobe of liver
5. Posteriorly: The lesser sac – which separates stomach from pancreas, transverse mesocolon, left renal and suprarenal gland, spleen and splenic artery
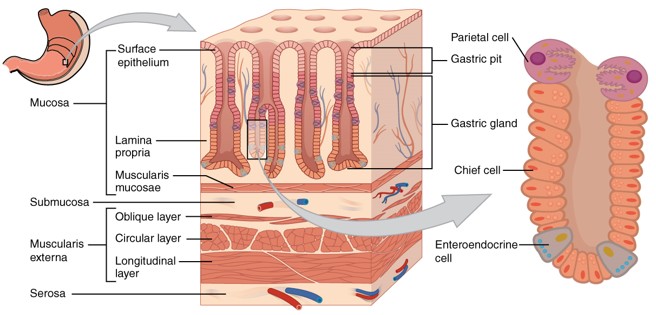
HISTOLOGY OF STOMACH (4 LAYERED WALL)
1. Mucosa:
- 3 sub-layers: mucous epithelium, lamina propria and muscularis mucosa (in to out)
- Arranged in a coarse rugal pattern
- Blood supply arises from rich vascular network of submucosa
2. Submucosa
3. Muscularis:
- 3 layers: outermost longitudinal, middle circular and innermost oblique layer
- Gastric pacemaker in fundus is located in middle circular layer
4. Serosa or Visceral peritoneum
Since, stomach contains 3 layers of smooth muscle in muscular layer, it is the most common site of GIST which is thought to be a leiomyoma.
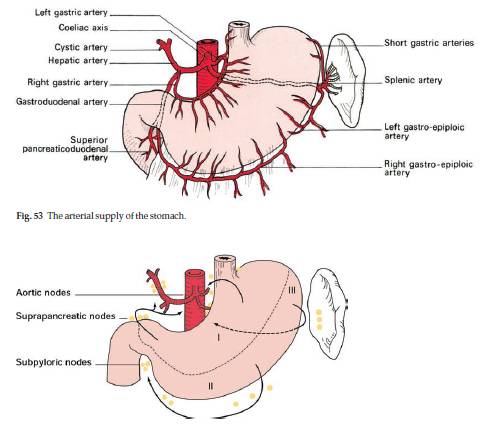
ARTERIAL SUPPLY OF STOMACH
At the lesser curvature: Anastomosis of –
- Left gastric artery (from Celiac axis)
- Right gastric artery (from Hepatic artery which is a branch of celiac axis)
At the greater curvature: Anastomosis of –
- Left gastro-epiploic artery (from Splenic artery)
- Right gastro-epiploic artery (from Gastroduodenal branch of Hepatic artery)
To the fundus: 5-7 short gastric arteries or Vasa-brevia (from splenic artery)
Draw to know it – Branches of celiac trunk
Because of this abundant blood supply, unintended surgical devascularization of the stomach rarely occurs. Sympathetic innervation parallels arterial flow.
LYMPHATIC DRAINAGE OF STOMACH
Anatomical lymphatic drainage (note: not the lymph node stations)
Area I – superior 2/3rd of the stomach drain along the left and right gastric vessels to the aortic nodes
Area II – right 2/3rd of the inferior 1/3rd of the stomach drain along the right gastro-epiploic vessels to the subpyloric nodes and then to the aortic nodes.
Area III – left 1/3rd of the greater curvature of the stomach drains along the short gastric and splenic vessels lying in the gastrosplenic and lienorenal ligaments, then, via the suprapancreatic nodes, to the aortic group.
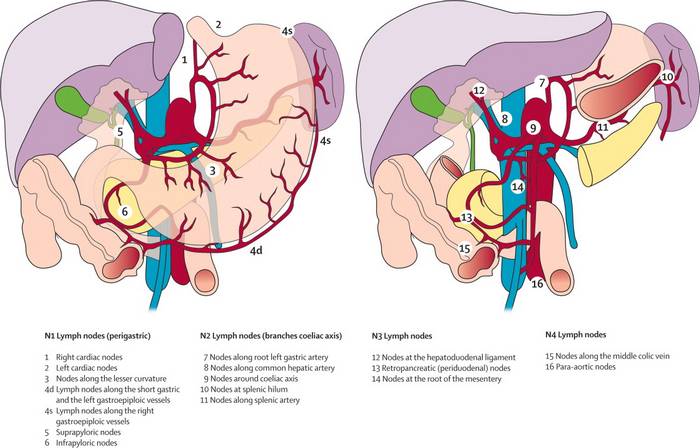
Gastric lymph node stations:
INNERVATION OF STOMACH
A. Intrinsic nerves:
- Myenteric plexus of Auerbach
- Submucosal plexus of Meissner
B. Extrinsic nerves:
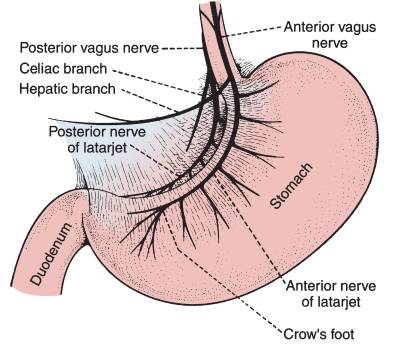
As the vagus nerve traverse the mediastinum, the left trunk rotates so that it enters the abdomen anterior to the esophagus and the right trunk rotates so that it enters posterior to the esophagus. The anterior and posterior vagi enter the abdomen through the esophageal hiatus on diaphragm. Vagus innervation constitutes both the motor and secretory nerve supply of the stomach.
- Anterior vagus nerve (Left vagus nerve) gives hepatic branch – passes through gastrohepatic ligament and innervates gallbladder, biliary tract and liver
- Posterior vagus nerve (Right vagus nerve) gives:
- celiac branch – runs along left gastric artery to celiac plexus from which nerve passes to midgut (pancreas, small intestine, and proximal colon as far as mid-transverse colon)
- criminal nerve of “Grassi” – supplies cardia of stomach (failure to divide this nerve may result in recurrent ulcer)
- Below these branches, both the vagus nerves continue down the lesser curvature as Anterior and Posterior nerve of Latarjet and give off side branches that innervate the stomach and terminal branches that innervate the pylorus (crow’s foot)
- Anterior vagus nerve – supplies cardia and lesser curvature
- Posterior vagus nerve – supplies both anterior and posterior aspects of body/corpus of stomach
- Crow’s feet innervation to antropyloric area: 2 main nerve trunks branch into multiple nerves at incisura forming crow’s foot, which innervates at antrum (preserved in highly selective vagotomy)
Almost 90% of vagus nerves are afferent (transmitting information from stomach to brain) and the rest 10% are efferent which pass without synapse to contact postsynaptic neurons in gastric wall in the myenteric and submucous plexus.
Mayo’s operation: Truncal vagotomy with posterior vertical retrocolic isoperistaltic no loop no tension gastrojejunostomy (drainage procedure); Heinke Mickulicz pyloroplasty can be used instead of gastrojejunostomy in truncal vagotomy
Selective vagotomy:
- Taylor procedure: Posterior truncal vagotomy with anterior lesser curve seromyotomy
- Hill procedure: Posterior truncal vagotomy + Anterior highly selective vagotomy
Highly selective vagotomy: Only the gastric branches (parietal cell) are cut preserving the nerve of Latarjet (crow’s foot) supplying the pylorus
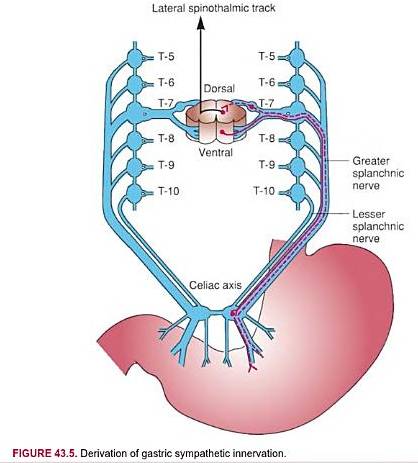
Sympathetic innervation:
- Spinal segment: T5-T10
- Presynaptic fibers pass through the greater splanchnic nerves to the celiac plexus, where they synapse with secondary sympathetic neurons. Postsynaptic sympathetic nerve fibers enter the stomach in association with blood vessels.
- Gastroduodenal pain is sensed by afferent fibers of sympathetic origin.
Gastric contractions are increased by parasympathetic stimulation and decreased by sympathetic stimulation. Even during fasting, migrating myoelectric complex (MMC) mediated by motilin occur at 90 minute interval and clear the stomach of residual food.
great details appreciated