Coronaviridae, one of the families of viruses which are known to cause diseases in mammals and birds ranging from the common cold to Severe Acute Respiratory Syndrome. A new species which belongs to this family emerged recently causing an outbreak of a respiratory disease in the eastern part of Asia.
Taxonomy of Coronavirus
- Order – Nirovirales
- Family – Coronaviridae
- Genus – Coronavirus
- Species –
- Human Coronavirus 229E
- Human Coronavirus OHuman Coronavirus NL63
- Human Coronavirus HKU
- SARS related Coronavirus (Sever Acute Respiratory Syndrome)
- MERS related Coronavirus (Middle East Respiratory Syndrome)
- Novel Coronavirus (CoViD – 2019)
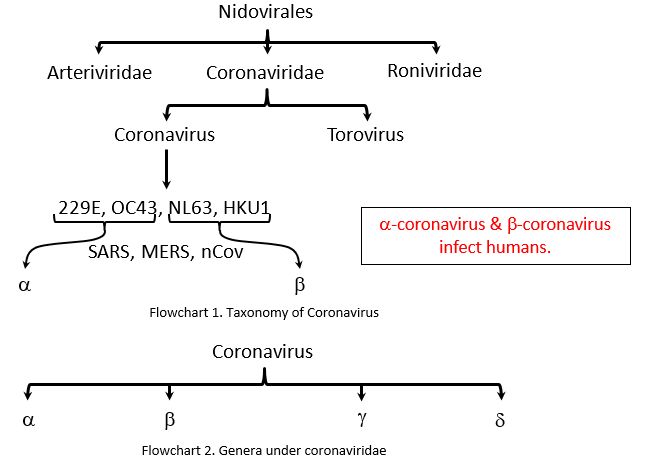
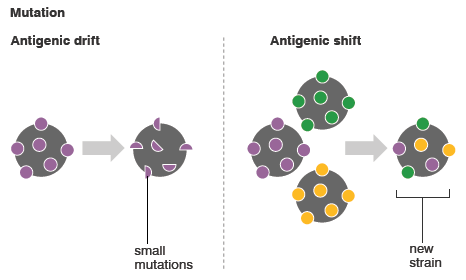
Evolution: The oldest ancestor i.e., MRCA (Most Recent Common Ancestor) for these group of viruses dates back to 8000 B.C., which was initially seen only infecting bats and birds. Due to industrialization, deforestation and their consumption of bats, birds and other animals as food by humans, it has also started to infect humans. The first species of Coronavirus infecting humans (229E) was identified in 1931 and isolated first in 1965. Eventually, the virus has evolved into the novel Coronavirus (2019-n-CoV).
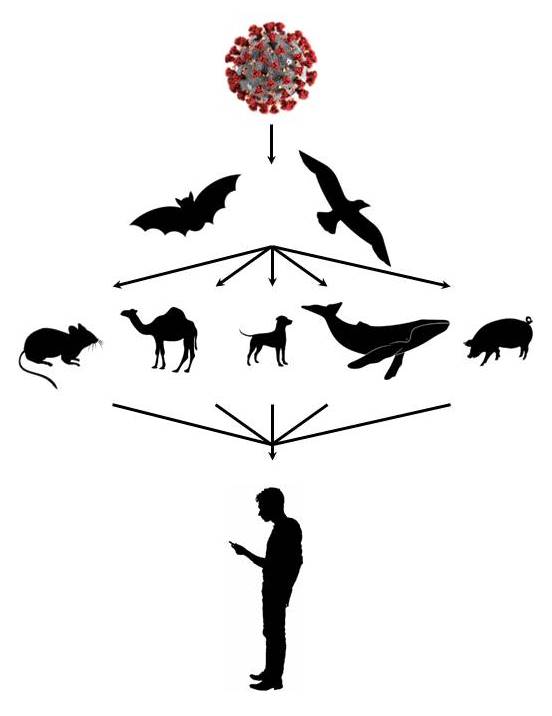
Flowchart 3. Spread of the virus in various hosts.
History of Serious Outbreaks caused by Coronavirus:
- 2002-03: SARS in China
- 2012: MERS in Saudi Arabia
- 2015: MERS in South Korea
- 2019-20: SARS CoV/nCov
Corona Virus
A single-stranded positive-sense RNA virus.
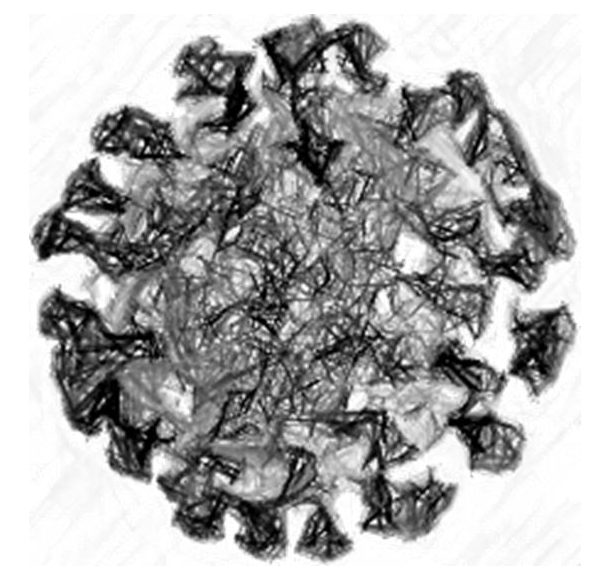
Spherical in shape, 80-160 nm in diameter, Helical Nucleocapsid, Enveloped (hence can be destroyed by organic solvents) with 12-24 nm spikes.
Major structural proteins: S-Spike, E-Envelope, M-Membrane, N-Nucleocapsid, HE-Hemagglutinin (seen only in HCoV-OC43 and SARS CoV).
Its Genome is considered the largest among the RNA viruses with 30,000 nucleotides.
Replicates in the cytoplasm of the host cell and obtains the envelope from the Golgi Apparatus/Endoplasmic Reticulum.
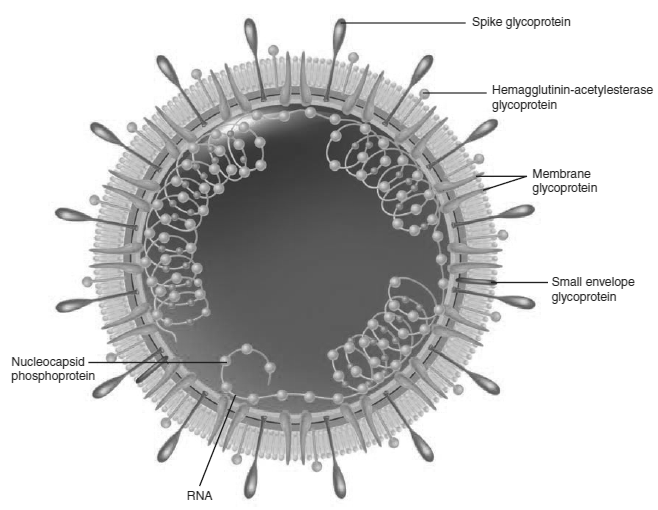
Fig 1. Structure of Coronavirus [5]
Corona Virus Disease (CoViD)
Clinical Presentation:
Human Coronavirus is known to produce common cold (running nose with malaise) which weans off by 1 week. It rarely causes lower respiratory tract infections.
SARS/MERS is known to cause severe lower respiratory tract infections such as severe pneumonia, moderate to severe ARDS (Acute Respiratory Distress Syndrome), sepsis, septic shock.
The virus can spread across the population by respiratory droplets.
Detection of a patient with Coronavirus Disease (Case Definitions):
The WHO after recognizing the coronavirus disease as a potentially dangerous one with an easy transmission has put forward few pointers for the health care workers to identify the suspects and bring them to better medical attention and care in the early stages of the disease.
The main objective of the definitions is to limit the spread of the disease in the population by identifying the potential suspects and isolating them.

Fig 2. Case Definitions (WHO)
Case Management at OPD:
An immediate Infection and prevention control has to be followed as soon as any patient meets the case definitions.
The patient has to be handed over a mask and instructed the correct method of using it. He/She needs to be isolated from other patients and needs to be educated about hand hygiene and respiratory hygiene.
Health care staff needs to be educated regarding mask management and hand hygiene.
Case Management at ICU/Ward:
Categorize the patient based on the symptoms to place them in an ICU or a Ward.
Start supplemental oxygen therapy to patients with respiratory distress.
Manage fluid and electrolyte balance if the patient presents with SARI (Severe Acute Respiratory Infection)and not in shock.
Administer empiric antimicrobials against likely pathogens causing SARI.
Counsel the patient and the relative regarding the disease and the probable course of management.
Laboratory Diagnosis:
Specimen – Respiratory material from URT (nasopharyngeal and oropharyngeal swab/secretions) and LRT (sputum, endotracheal aspirate or bronchoalveolar lavage), blood samples and serum.
Investigations – NAAT (Nucleic Acid Amplification Test) and RT-PCR (Reverse Transcription Polymerase Chain Reaction) to be done on the respiratory secretions, blood culture may be done to rule out other aetiology causing a similar pattern of illness. If NAAT and PCR are not available tests on serum can be done to evaluate the host immune response.
A regular investigation panel has to be carried out on a confirmed patient until 2 consecutive samples are negative taken 24 hours apart only when clinically recovered.
THE PATIENT HAS TO BE MONITORED CLOSELY TO PREVENT DETERIORATION, ON THE CONTRARY, IF THE PATIENT IS SEEN WORSENING ADEQUATE SUPPORT HAS TO BE GIVEN.
Prevention:
General Precautions –
Get to know the various presentation of the disease, maintain a distance of 1m from an infected person as it is a respiratory disease. Maintain hand and respiratory hygiene. Get medical attention as soon as possible if you can identify the symptoms.

Fig 3. Precautions to be taken by one
Hand Hygiene – Has to be performed regularly, with wither alcohol-based solution or soap (if hands are visibly soiled). It has to be done strictly if there has been contact with an infectious individual. Use disposable towels or napkins after the wash.
Respiratory Hygiene – If one is sick with any respiratory symptoms, he/she has to try to isolate themselves as much as possible. Cover your mouth and nose properly during a sneeze or cough followed by washing hands thoroughly. Use a surgical mask.
Duties of the Hospital Management Team –
Hospitals are a hub of infected patients in such a situation and a lot of care has to be taken to limit the spread.
Any diagnostic procedure on these patients has to be preceded and followed by stringent guidelines and precautions. These procedures have to be conducted in a HEPA (High Efficiency Particulate Air) filter rooms or AIIR (Airborne Infection Isolation Room).

Fig 4. Precautions at a Health Care Set-Up
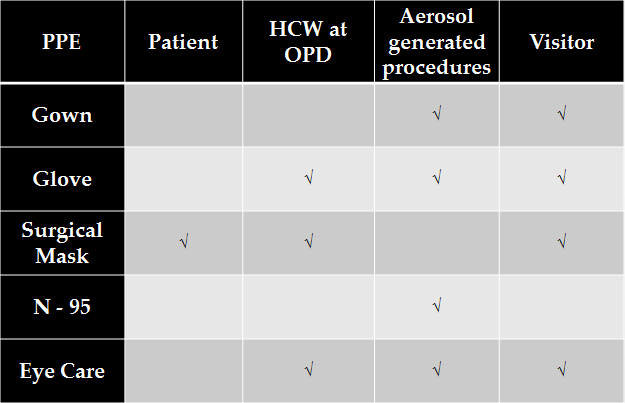
Table 1. Personal Protective Equipment
Maintenance of the Hospital –
A strict policy has to be designed by the hospital authority to curb the mode of spread. Disinfection needs to be carried out using 70% Ethyl Alcohol or 0.5% Sodium Hypochlorite.

Fig 5. Measures to prevent further transmission
Laboratory Measures
Highly infectious material is handled at the labs for investigation, which makes it a potentially serious threat for transmission. Stringent standards have to be maintained by the laboratories. Specific samples have to be handled in designated level laboratories (Biosaftey Level).
Non-propagative work (NAAT, PCR) in a BSL– 2
Propagative work (Culture) in a BSL – 3

Fig 6. Laboratory Safety.
Summary
Coronavirus named due to its resemblance to SUN which contains the largest genome among RNA viruses.
It usually causes respiratory illness and rarely gastrointestinal symptoms too.
The virus initially was identified in bats and birds and due to increased interaction and consumption, it is seen that humans are also infected.
Adequate measures have to be taken by all the sectors of society to prevent further transmission of the disease. This initiative has to be taken not only by the hospital management and policymakers but also by the citizens.
Measures are to be taken such as preventing close contact with the infected individual, maintaining hand and respiratory hygiene. Use a correct mask at the correct time in the right place following adequate guidelines.
References
- World Health Organization Website – https://www.who.int/emergencies/diseases/novel-coronavirus-2019
- Center for Diseases Control Website – https://www.cdc.gov/coronavirus/index.html
- Jawetz Medical Microbiology, Coronavirus.
- Virology, An Illustrated Color Text, Stephen Korsman, Human Coronaviruses.
- Sherri’s Medical Microbiology, Coronaviruses.
- Schaechter’s Mechanism of Microbial Diseases, Coronavirus, SARS.

Graduated from one of the famous institutions in Telangana, Kamineni Institute of Medical Sciences. He has always been fond of writing articles in Medicine. Since the undergraduate years was interested in making creative Presentations and taking seminars.
We appreciate for explaining the Evolution of Caronavirus in detail. Thank you for the Precautions to be taken to fight against COVID.
This blog article is very important for people in the present situation.
Thank you Kumar. Hope you have shared this article with as many as possible to stay safe.
Thanks, for this post really helpful. I think the article does a wonderful job of underscoring the importance. The COVID-19 pandemic has impacted several hospitals across the globe. This article appropriately explains the volatility of the healthcare industry at the moment in relation to hospitals.