Myiasis is defined as the infestation of live vertebrates (humans and/or animals) with dipterous larvae. The order Diptera is a large order of insects that are commonly known as true flies. Myiasis may be classified clinically into:
- Furuncular (subcutaneous) myiasis
- Wound (superficial cutaneous) myiasis
- Cavitary (atrial or invasive) myiasis
- Intestinal myiasis
- Urinary myiasis
- Vaginal myiasis
Wound myiasis occurs when fly larvae infest open wounds of a mammalian host. Majority of flies that are likely to cause myiasis in humans belong either to the blowfly group, family calliphoridae, or the housefly group, family muscidae. Myiasis is mostly accidental or opportunistic, but may also be purposeful, or obligate, with the maggots requiring time inside host tissues for development. Except for obligate cases (e.g., screwworm fly or bot fly), myiasis is generally not life-threatening.
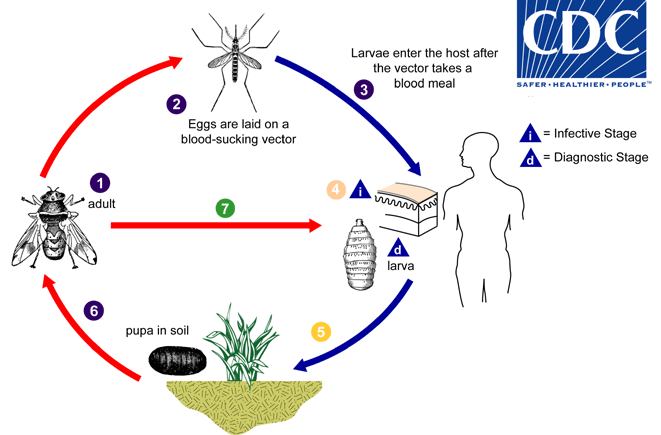
Lifecycle of Maggot
- Flies are attracted to open or infected wound and the female flies lay 50-300 eggs on wound (about 1.7 mm long) at a time.
- These hatch around 8-12 hours later (emerging larvae are also about 1.7 mm long) at skin temperature.
- Within 24 hours, they grow upto 7-8.5 mm long and in 50-60 hours, larvae attain full growth.
- Then, they migrate to dry crevice or soil to pupate.
Fly larvae are not capable of reproduction, and therefore, myiasis should not be considered contagious from patient to patient. Transmission of myiasis occurs only via an adult female fly.
Causal agents of Wound myiasis
- Cochliomyia hominovorax (New world screwworm)
- Chrysomya bezziana (Old world screwworm)
- Wohlfahrita magnifica (Old world fleshfly)
- Dermatobia hominis (Human botfly)
- Musca domestica (Housefly)
- Others: Chrysomya megacephala, Calliphora vicina, L. sericata, Chrysomya albiceps, Phormia regina, Parasarcophaga argyrostoma, Lucilia cuprina, and Sarcodexia lambens
Diagnosis of Wound Myiasis
Often the clinical diagnosis is clear-cut with visible larvae in the mal-odorous and bleeding/discharging wound.
Greenberg identified 4 risk factors for maggot infestation:
- Helpless or debilitated person
- Bleeding or odors of decomposition present
- Summer season
- Neglect in nursing care
It is recommended that a maggot should be submitted to the laboratory in alcohol or formaldehyde and at least one maggot should be submitted alive to facilitate species identification.
Treatment of Wound Myiasis
- Removal of all visible larvae. Care should be taken to avoid lacerating the larva because retained larval parts may precipitate foreign body reaction.
- Debridement in cases where necrotic tissue still remains
- Antibiotics for secondary infections
- Irrigation may be useful for lesions with holes and cavities.
- 15% chloroform in olive oil or another oil or ether may help to immobilize the larvae and facilitate maggot removal. The use of a thick layer of petrolatum, with its removal every 3 h until the complete removal of the larvae is achieved, is also an option. These work by asphyxiating the larva and compelling them to come out of the wound.
- Topical and Oral ivermectin have also been used successfully.
Depending on the wound, surgical removal may not be required unless requested by the patient, as the larvae are naturally sloughed within 5-7 weeks.
References:
- Francesconi F, Lupi O. Myiasis. Clin Microbiol Rev. 2012 Jan;25(1):79-105. doi: 10.1128/CMR.00010-11. PMID: 22232372; PMCID: PMC3255963.
- Predy G, Angus M, Honish L, E Burnett C, Stagg A. Myiasis in an urban setting: A case report. Can J Infect Dis. 2004 Jan;15(1):51-2. doi: 10.1155/2004/978427. PMID: 18159443; PMCID: PMC2094924.
- Sunny B, Sulthana L, James A, Sivakumar T. Maggot Infestation: Various Treatment Modalities. J Am Coll Clin Wound Spec. 2018 Mar 30;8(1-3):51-53. doi: 10.1016/j.jccw.2018.03.002. PMID: 30276127; PMCID: PMC6161638.
- https://emedicine.medscape.com/article/1491170-treatment
I find the treatment section especially useful.