Proptosis refers to the forward displacement of the eyeball beyond the orbital margin with the patient looking straight ahead. The term “Exopthalmos” is reserved for bilateral proptosis or proptosis due to thyroid eye disease. Proptosis can be evaluated using a mnemonic 15 “P”s.
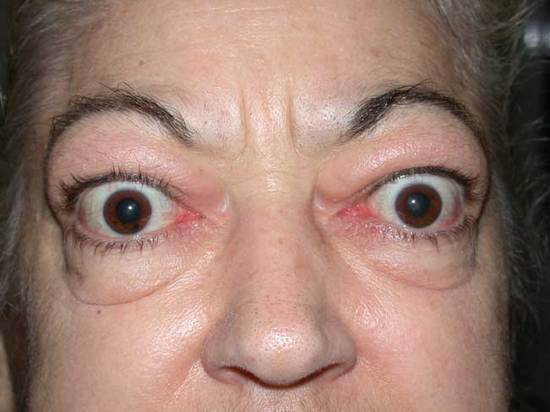
A) Pseudoproptosis ruled out:
1. Enlarged globe:
- Congenital bupthalmous
- High axial myopia
- Staphyloma
- Unilateral seconday glaucoma in childhood
2. Lid retraction:
- Microblepharon
- Dermatosis or icthyosis or from scarring
- Sympathetic overaction like Grave’s disease or Parkinson’s disease
3. Lower lid sagging:
- Facial palsy
- Retraction of inferior rectus
- Following recession of inferior oblique
4. Deformation of orbit or facial asymmetry:
- Asymmetry of bony orbit
- Progressive facial hemiatrophy (Parry-Rombergs’ syndrome)
- Harlequin orbit
- Hypoplastic supraorbital ridges as in trisomy 18
- Shallow orbit as in Crouzon’s disease (craniofacial dysostosis)
5. Opposite eye enophthalmos
B) Pain
Painful conditions are:
a. Infection and Inflammatory conditions: Orbital cellulitis, Orbital abscess, Orbital pseudotumor, Myocysticercosis
b. Vascular condition: Lymphangioma, High flow carotid-cavernous fistula
c. Metastatic lesion
d. Malignant lesion: Retinoblastoma, Rhabdomyosarcoma
e. Trauma
f. Thyroid orbitopathy
C) Progression
a. Acute (hours to a week): Infection, Inflammation, Parasitic infestation, Trauma, Metastatic lesions or Lymphangioma
b. Subacute (1-4 weeks): Inflammation, Parasitic infestation or Metastatic lesions
c. Chronic (> 4 weeks): Thyroid associated orbitopathy, Orbital varices, Benign neoplasia (Cavernous hemangioma, Neurofibroma, Schwannoma, Glioma of optic nerve)
D) Proptosis type
1. Axial proptosis: displacement of the globe horizontally forward from its usual position, suggests retro-ocular pathology such as an orbital apex mass or muscle swelling.
- Optic nerve glioma
- Cavernous hemangioma
- Meningioma
- Schwanomma
- Metastatic tumors from CA—breast, lung or prostate
2. Non-axial proptosis: globe is displaced not only forwards but also away from its usual axis, suggests a mass arising from elsewhere in the orbit.
Down & out:
- Fronto-ethmoidal lesions
- Supero-medial space lesions: Dermoid, Hemangioma
Down & in:
- Lacrimal gland pathology
- Lacrimal fossa lesions: Dermoid
Upwards:
- Maxillary sinus lesions
- Inferior space lesions: Cavernous hemangioma, neurofibroma, schwannoma, neurocysticercosis of inferior rectus
E) Position
Unilateral: Thyroid orbitopathy, Inflammatory lesions, Vascular lesions, Cysts, Tumors, Trauma, Leukemia, Localized amyloidosis
Bilateral: Thyroid orbitopathy, Craniofacial dysostosis, Encephalocele, Carotid sinus thrombosis, Nasopharyngeal malignancy
Commonest cause of unilateral or bilateral proptosis in adults: Thyroid orbitopathy
Commonest cause of unilateral proptosis in children: Orbital cellulitis
F) Pulsations
Vascular pulsation: Carotid-cavernous fistula (CCF), Carotid sinus thrombosis, Vascular tumors (hemangioma)
Transmitted (Cerebral) pulsation (due to orbital wall defect): Neurofibroma, Meningo-encephalocele
Auscultate for bruit to detect high-flow CCF
G) Periodicity
Intermittent proptosis is seen in:
- Orbital varices (90%)
- Highly vascular neoplasms like hemangioma or lymphangioma
- Recurrent orbital hemorrhages
- Intermittent ethmoiditis
H) Pupils
Presence of RAPD indicates Optic nerve damage:
- Optic nerve/sheath tumors
- Compression due to space occupying lesions of central space
- Compression due to enlarged extraocular muscles (thyroid orbitopathy)
- Compression due to non-specific inflammation in orbit
I) Provocative examination (Valsalva maneuver)
Increase in proptosis on valsalva maneuver is seen in Orbital varix.
J) Perception of Color Vision
Assessment of Optic nerve function in following situations:
a. In Early optic nerve compression: VA can be 20/20, fundoscopy may be normal and Visual field may be normal
b. In Bilateral lesions: RAPD may not be elicited
K) Prism Bar Cover Test (PBCT)
When there is limtation in ocular motility:
1. Differentiate if pathology is restrictive or paralytic:
a. Forced Duction Test (FDT) positive: Resistance when globe tried to move in the direction of restriction
b. Differential tonometry: Increase in IOP > 5 mmHg when patient tries to move globe in the direction of restriction
2. Quantify with PBCT or Hirschberg test
L) Peri-orbital changes
- Salmon colored mass in inner part of eyelid: Lymphoma
- Eyelid retraction and eyelid lag: Thyroid eye disease
- Vascular congestion over insertion of rectus: Thyorid eye disease
- Corkscrew conjunctival vessels: AV fistula
- Vascular anomaly of eyelid skin: Lymphangioma, varix, capillary hemangioma
- S-shaped eyelid: Neurofibroma, Lacrimal gland mass
- Eczematous lesions of eyelids: T-cell lymphoma
- Ecchymoses of eyelid skin: Metastatic neuroblastoma, leukemia, trauma
- Prominent temporal bone: Sphenoid wing meningioma, Metastatic neuroblastoma
- Edematous swelling of lower lid: Meningioma, Inflammatory tumor
M) Palpation
Palpable mass
Retropulsion
Crepitus: Orbital emphysema (communication between orbit and sinus)
N) Proptometry
Naphzeiger’s test: Ask the patient to look at a distant object, located at the same level as that of the patient’s eye. Stand behind the patient, and gently tilt the head backwards and look down over the patient’s forehead. The proptosed eye appears ahead of the other.
Using ruler: Space between a scale from middle of Superior orbital to Inferior orbital margin and Eyelids is obliterated in proptosis.
Exophthalmometer (hertel’s): Normally, the corneal apex is less than 20 mm from the lateral bony orbital margin and there is usually 2 mm or less difference between the two eyes.