Pattern of bone loss in Osteoporosis
- Trabecular bone responds faster to metabolic changes due to greater surface are compared to cortical bone.
- Non-weight bearing (secondary trabeculae) are lost first. Weight bearing (primary trabeculae) may appear prominent due to loss of other trabeculae and may also become thickened due to compensatory mechanism or callus from microfractures.
- Later, even primary weight-bearing trabeculae are lost, resulting in translucent appearance of bone.
- In bones that sustain vertical loads, such as tibial and femoral metaphyses and vertebral bodies, resistance to lateral bowing and fractures is provided by a horizontal trabecular cross-bracing system that helps support the vertical elements.
Trabeculae in Proximal Femur
5 groups based on orientation and function:
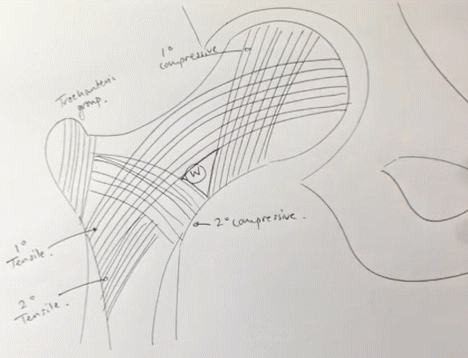
- Primary compressive group
- Secondary compressive group
- Greater trochanteric group
- Primary tensile group
- Secondary tensile group
How do you remember where these trabeculae are ?
I use these general rules:
- Primary trabeculae start in head of femur as they are weight-bearing trabeculae.
- Secondary trabeculae lie inferior to the primary trabeculae.
- Compressive trabeculae go towards compression side of the proximal femur, i.e. medial side with lesser trochanter.
- Tensile trabeculae go towards tension side of the proximal femur, i.e. lateral side with greater trochanter.
- Greater trochanteric group is confined within greater trochanter.
Ward triangle refers to a radiolucent area between principal compressive, secondary compressive and primary tensile trabeculae in the neck of femur. This is the area having lowest BMD in femoral neck.
Singh’s Index
Based on the loss of trabecular pattern in proximal femur, Singh index is used to assist fracture prediction. As described by Singh index, trabecular bone loss in osteoporosis initiates in the trochanter, then evolves to the breakage of tensile trabeculae, and ultimately reaches the principal compressive trabeculae.
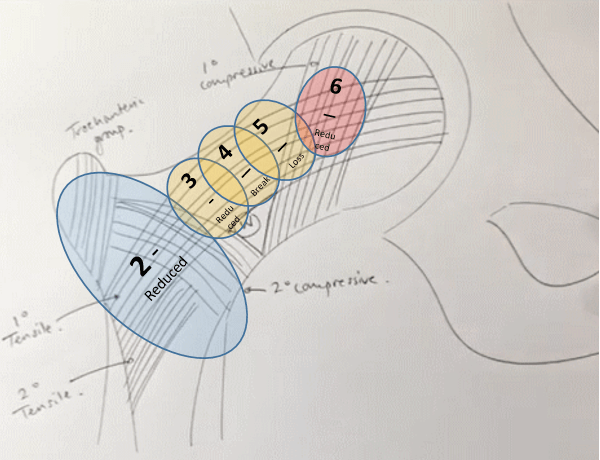
Grade 6 – All normal trabeculae groups visible
Grade 5 – Reduction/Loss of trochanteric and secondary trabeculae leading to: prominence of primary groups and enlargement of Ward’s triangle
Grade 4 – Reduced but continuous primary tensile group
Grade 3 – Discontinuous primary tensile group
Grade 2 – Loss of primary tensile group as well (Only primary compressive group visible)
Grade 1 – Reduction in primary compressive group
However, Singh’s index has been found to poorly correlate with the BMD measured using DEXA or quantitative CT scan.

He is the section editor of Orthopedics in Epomedicine. He searches for and share simpler ways to make complicated medical topics simple. He also loves writing poetry, listening and playing music. He is currently pursuing Fellowship in Hip, Pelvi-acetabulum and Arthroplasty at B&B Hospital.
What is the name of the person in Singh sintex ? Who is Singh ?
Dr. Manmohan Singh (Orthopedician) seems to be eponymous researcher behind the Singh’s Index.
Singh M, Nagrath AR, Maini PS. Changes in trabecular pattern of the upper end of the femur as an index of osteoporosis. J Bone Joint Surg Am. 1970 Apr;52(3):457-67. PMID: 5425640.