A) Cardiovascular complications
1. Exacerbation or Precipitation of CHF – Voluminous AV Fistula
AV shunting → Decreased TPR → BP fall → Sympathetic stimulation & RAAS activation → Ventricular remodeling → Heart failure
Several studies have investigated the cut-off fistula access flow that is associated with a higher risk of high-output cardiac failure, with results ranging between 1.5 and 2.0 l/min
Requires surgical management of AV defect
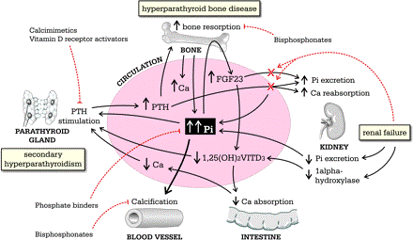
2. Vascular and Cardiac calcifications –
- 2⁰ hyperparathyroidism
- Ca²⁺ containing binders
- Vitamin D analogues
3. Exacerbation of hypertension – Erythropoiesis Stimulating Agents (ESA)
ESA mediated increased TPR is mediated by increase in endothelins, angiotensin, impaired vascular entothelial relaxation, altered calcium levels in vascular smooth muscle cells and the release of serotonin by the platelets.
4. Hyperhomocysteinemia: defined as a plasma total homocysteine level of 12 µmol/l
5. Inadequate Intradialysis Ultrafiltration (UF)
6. Rapid electrolyte changes during dialysis session
7. Hyperlipidemia and accelerated atherosclerosis
8. Dialysis pericarditis, endocarditis
- Endocarditis – S.aurueus, 20%, poor prognosis, ageing + valve calcification
B) Gastrointestinal Complications
1. Anorexia and Nausea – Reduced dialysis dose
Anorexia has been attributed to the increase in leptins.
2. Gastritis and GI bleeding risk –
- Heparin during HD (Hemodialysis)
- Drugs stimulating gastric acid secretion
- Severe 2⁰ hyperparathyroidism
3. Hypercalcemia
4. Colonic diverticulosis – esp. in PKD
5. Ascites – Chronic volume overload
6. Angiodysplasia: submucosal capillary dilation and fibromuscular hyperplasia; important cause of EPO resistant anemia; treatment is APC (Argon Plasma Coagulation)
7. Hemosiderosis – Excessive transfusion
Note: Hemosiderosis (reversible) vs Hemochromatosis (irreversible)
8. Constipation
- Iron
- Ca²⁺ containing binders
9. Laxative effects – Other phosphate binders
10. Pseudomembranous colitis – prolonged antibiotics
C) Anemia
1. Chronic hemolysis:
- Direct traumatic effect – dialysis circuit
- Toxic substances in dialysate – Cu, NH2Cl, NO3, Zn, Fl
- Abnormal changes of temperature/osmolarity of dialysate
2. Iron deficiency:
- Reduced intestinal absorption
- GI or GU hemorrhages
- Blood loss in dialysor and dialysis circuit
- Repeated venipuncture – repeated lab tests
3. Folate deficiency:
- Poor intake
- Loss through dialysis membrane
4. Endogenous EPO synthesis inhibition – Repeated transfusions
5. Aluminium toxicity:
- Al-based phosphate binders
- High Al concentration in dialysate
- Al inhibits heme synthesis
- Prevented by reverse osmosis (RO) of water
6. Myelofibrosis- Severe 2⁰ hyperparathyroidism
D) Erythropoiesis stimulating agents (ESA) associated complications
1. Hypertension – onset or worsening
2. Vascular access thrombosis
3. Erythrocytosis
4. Aplastic anemia
Platelets Increased production of microparticles Enhanced platelet activation Vascular endothelium Mitogenic, chemotacticy and angiogenic effect Increased endothelin production Increased PAI-1 production Vascular smooth muscle Raises cytosolic Ca2+ concentration Increases responses to norepinephrine, angiotensin II, and endothelin-1 Mitogenic effect Cardiomyocytes Enhances proliferation (neonatal) Stimulates Na+,K+ activity
E) Bleeding Diathesis
1. Blood – Dialysor contact:
- Platelets or monocyte activation
- Release of cytokines and NO
2. Heparin during HD:
- ↑BT
- HIT (Heparin Induced Thrombocytopenia)
3. Antiplatelets – Vascular patients
4. GI bleeding in HIV associated nephropathy: Kaposi’s sarcoma, NHL, CMV colitis
5. With PAN – Spontaneous retroperitoneal bleeding
6. Oral anticoagulants or Severe HTN – Intracerebral hemorrhage
F) Pulmonary Complications
1. Pulmonary infections
- Depressed immunity
2. Pleural effusion
- Chronic inadequate dialysis dose
- Heparin – Hemorrhagic
- Exclude other causes –
- Infections (Viral/Bacterial)
- Systemic causes
- CHF
- Severe hypoproteinemia
G) Bone Disorders
1. Adynamic bone disease – Excessive vitamin D3
- Diabetic nephropathy
- Vit D hypersecretion & hypercalcemia – Granulomatous disease (TB, sarcoidosis, etc.)
2. Aluminum bone toxicity – Low bone turnover:
- Contaminated dialysate and Al-based phosphate binders
- Sodium citrate therapy for metabolic acidosis
3. Non-aluminum osteomalacia:
- Negative calcium balance (reduced intake, low dialysate concentration)
- Long-standing metabolic acidosis (Tubulointerstitial nephropathy)
4. Dialysis amyloidosis:
- Atleast 5-7 years on dialysis
- Osteoarticular deposition of β2-microglobulin
- Stimulate osteoclastic bone resorption
Hemofiltration or high-flux hemodialysis to remove 2-microglobulin can be considered.
H) Neurologic complications
1. Dialysis dementia
2. Subdural hematoma
3. Wernicke acute encephalopathy (thiamine deficiency)
4. Encephalopathy 2⁰ to biotin deficiency
5. Mononeuropathy – Median nerve compression
- Amyloidosis
- Voluminous AV Fistula
- Steal syndrome – 2⁰ nerve ischemia
6. Iatrogenic complications:
- CN VIII damage – Aminoglycoside or Erythromycin
- Myositis – Clofibrate, Colchicine, Prednisone
7. Inter- or Intra-dialytic electrolyte imbalance:
- Muscle cramps – Hyponatremia
- Seizures – Hyponatremia
- Myositis – Hypophosphatemia
I) Carbohydrate metabolism
1. Hypoglycemia risk maintained:
- Severe 2⁰ hyperparathyroidism
- Malnutrition
2. Decrease in insulin need:
- HD restores peripheral resistance to insulin
3. Increase in insulin need:
- HD normalizes the half life of insulin
J) Protein metabolism
1. HD – catabolic process
- Protease release from erythrocytes
- Amino acid loss
- Hypoglycemia with glucose-free solutions
2. Decreased plasma creatinine in chronic HD:
- Not a marker of efficient dialysis
- Marker of malnutrition
- Associated with: hypoalbuminemia, decreased protein synthesis, reduced muscle mass
5 to 8 g of free amino acids per dialysis session with low-flux dialyzers 30% greater amino acid losses with high-flux dialyzers
Uremia is a hypercatabolic state; factors involved are: low protein intake, increased plasma hypercatabolic hormones that are insufficiently degraded by the kidney (glucagon, cortisone, catecholamine), tissue resistance to anabolic hormone actions as a result of accumulation of uremic toxins. Hemodialysis largely corrects these problems by removal of the toxins, normalizing the half-life of catabolic hormones and also by allowing a normal or hyperproteic diet
K) Lipid Metabolism
1. Type IV Hyperlipoproteinemia in CKD
- ↑VLDL, ↑IDL, ↓HDL
- Decreased activity of hepatic lipase and lipoprotein lipase
- Inhibitory effect of uremic toxin, Hyperinsulinism
- 2⁰ hyperparathyroidism, Excessive dietary fats
2. HD – doesn’t correct; may aggravate
- HDL lost at blood-dialysor
- High TGs – Heparin
3. More pronounced in – DKD and Nephrotic syndrome
L) Cutaneous manifestations
1. Pruritus
- 2⁰ hyperparathyroidism
- ↑ serum serotonin and histamine
2. Xerosis
- Perspiratory gland dysfunction
- Hypervitaminosis A, Hyperparathyroidism
3. Pigmentations
- Pallor – Anemia, Urochromes, Carotenoids
- Brown – Melanotropic hormone accumulation
4. Cutaneous calcifications – 2⁰ hyperparathyroidism
5. HD-associated bullous dermatitis:
- Allergic reaction to dialysate chemicals
- Drugs – Furosemide, Tetracycline, Nalidixic acid
M) Gonadal functions
1. Improved sexual function in male – without increase in testosterone
2. Reappearance of menstruation in females – but anovulatory cycles
3. Subfertility – rarely become pregnant
4. Rarely, carry pregnancy to term:
- Spontaneous abortions
- IUFD
- Premature births
- Pre-eclampsia
N) Vitamins
1. Causes of deficiency – Water soluble vitamins:
- Poor intake
- Loss from dialysor
2. Supplementation:
- Vitamin D
- Others – only from dietary intake
O) Immunological functions
1. T-lymphocyte activation → ↑APCs and IL-2 → Worsening of inflammatory state
- Blood – Dialysor interaction
2. Depressed normal antibody reactions
3. ↑ Increased autoantibody and anti-ethylenoxid antibodies
- Blood – Dialysor interaction
4. Neutrophilic and Complement activation – Protease and ROS release:
- Blood – Dialysor interaction (reduced biocompatibility)
- Platelet and RBC dysfunction
- Increased serum lipid peroxidation products
- ROS – amyloid arthropathy
- DNA distortion – premature aging
- Increased expression of adhesion molecules – Leucopenia
P) Viral Infections
1. Hepatitis B and C
- Increased risk
- Intravenous treatment
- Transfusions
2. HIV
- Comparable to general population
Q) Acquired Polycystic Kidney Disease
1. Associated with:
- Improvement of anemia
- Decreased erythropoietin need (EPO secretion in cystic walls)
2. Increased risk of – urothelial neoplasia
R) Complications induced by Primary Renal Disease
1. Rapid decline of residual renal function:
- Persistence of urinary excretion of TGF-β1:
- Diabetic glomerulopathies
- Idiopathic membranous glomerulopathies
- Nephrotic proteinuria:
- DKD
- Mesangiocapillary GN, FSGS
- Amyloidosis
- ACE inhibitor therapy – Ischemic nephropathy or Severe atherosclerosis
2. Bone disease:
- Chronic Metabolic acidosis – Tubulointersitial disease
- Diabetic patients – Unknown mechanisms
- High incidence of 2⁰ hyperparathyroidism – Analgesic nephropathy
- Myeloma
- Granulomatous diseases
3. Reccurence and comorbidities:
- Worsening or continuation of Diabetic retinopathy
- Rapid cyclic changes in plasma osmolarity during hemodialysis
- Malnutrition in DKD
- Medication, diabetic associated gastroparesis, CHF
- Intradialytic hypotension
- Autonomous neuropathy and diastolic dysfunction.
- Continued cardiac and microvascular complications of DM
- Hemolysis, hyperparathyroidism,dyslipidemia,atherosclerosis
- 50% asymptomatic IHD
- Increased Risk of UTI
- Diabetic neuropathy
- Risks of therapy for lupus exacerbation
References:
Chronic complications in hemodialysis: correlations with primary renal disease I. A. CHECHERIŢĂ, FLAVIA TURCU, R. F. DRAGOMIRESCU, A. CIOCÂLTEU
Hemodialysis Complications - Jonathan Himmelfarb, MD