Table of Contents
Amidst the post-earthquake fear, we managed to complete our 15 days internship in the Dermatology department which was setup in the patient’s waiting hall. The posting went pretty well; the learning experience was fun – thanks to the teachers and seniors who provided us with friendly environment and guidance. A variety of cases were seen and managed but the commonest cases encountered were:
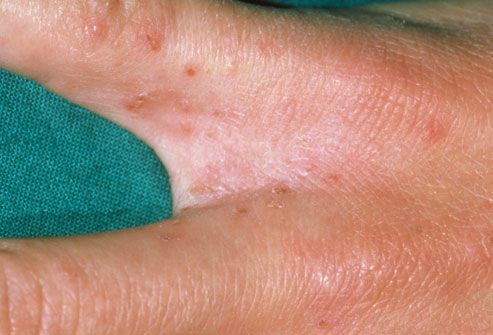
A) SCABIES
Causative organism: Sarcoptes scabiei (Mite) – Approximately 40–50 eggs are laid by each female during a lifespan of 4–6 weeks.
Spread: Prolonged and intimate contact (also considered as a sexually transmitted infection)
Cardinal features for diagnosis of scabies:
- Morphology: Burrows – linear tunnel in which the mite lives and appears as slightly elevated, grayish, tortuous lines in the skin. A vesicle or pustule containing the mite may be noted at the end of the burrow. To identify burrows quickly, a drop of India ink or gentian violet can be applied to the infested area, then removed with alcohol. Thin threadlike burrows retain the ink.
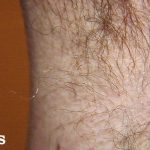
- Sites of involvement: An imaginary circle intersecting the main sites of involvement—axillae, elbow flexures, wrists and hands, and crotch—has long been called the circle of Hebra. Scalp and face are commonly uninvolved in adults – the mites appear to avoid areas with a high density of pilosebaceous follicles.
- Symptom: Itching which is severe at night. Pruritus occurs due to hypersensitivity – Evidence suggests that both immediate and delayed-type hypersensitivity are involved (itching can persist for weeks after the lesions disappear).
- Spread: Itching and similar lesions in family members. Naive individuals may be asymptomatic for 4-6 weeks.
Types and secondary changes of scabies:
- Nodular scabies
- Norwegian scabies (Crusted lesions with frequent nail involvement seen in immuno-compromised patients)
- Scabies incognito (Typical lesions modified by the use of steroids)
- Bullous pemphigoid-like eruption
- Others: Secondary infection, Eczematization
Treatment:
- Scabicidal agent: A single application of Permethrin (Permiriv) 5% applied to the whole body below the jawline before sleeping (for 8-10 hours before it is washed) is the treatment of choice. All family members must be treated simulatneously. Ivermectin (Iver-DT) 200 μg/kg is an oral scabicidal agent used in conjunction with Permethrin in cases of Norwegian scabies. It may need to be repeated 2-3 times at intervals of 1–2 weeks.
- Other scabicidal agents: Benzyl benzoate 25%, Gamma BHC 1% (Avoid in infants), Crotamiton 10%, Precipitated sulphur 10%
- Anti-pruritic: Antihistaminics like Levo-cetrizine (Levocet) 5 mg (2.5 mg for children) are often prescribed for 5-7 days to be taken before sleep as they cause sedation.
- Others: Laundering of bed sheets and treatment of all clothings
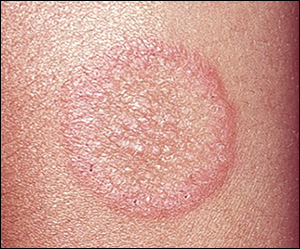
B) TINEA (DERMATOPHYTOSIS)
Causative organisms: Dermatophytes – Trichophyton, Microsporum, Epidermatophyton. Zoophilic species tend to produce highly inflammatory reactions in humans and this may lead to a spontaneous cure. Anthropophilic species produce mild but chronic lesions.
Morphology:
a. Prototype lesion: Itchy, annular/arcuate polycyclic lesion with clear center and an active margin of papulovesicles and scaling.
b. Scalp lesion: Frequently these lesions are to be differentiated from the alopecia areata. Though both manifest as noncicatricial alopecia, in contrast to the later, tinea capitis mainly occurs in children and is characterized by easily pluckable hairs.
c. Tinea incognito: Lesions modified by steroid therapy (Cloben-g is one such over the counter medication)
Sites:
- Tinea capitis (Scalp): Microsporum canis
- Non-inflammatory: Grey/black dots
- Inflammatory: Kerion (boggy swelling with pustules) and Favus (yellowish cup-shaped crusts entangling scalp hair with distinctive mousy odour)
- Tinea corporis (Glaborous skin of trunk)
- Tinea faciei (Face): Trichophyton rubrum
- Tinea barbae (Beard)
- Tinea cruris (Groin): T.rubrum
- Tinea pedias (Foot): Variants – Interdigital (Athlete’s foot), Hyperkeratotic (Scaly) and Vesicular
- Tinea unguim (Nails): Onycholysis, Subungual hyperkeratosis and Tunneling
- Tinea manuum (Hands): Trichophyton erinacei
- Tinea imbricata (Tokelau)
Diagnosis: When the diagnosis is not certain and needs to be differentiated from other papulosquamous lesions like psoriasis or eczema – treatment can be initiated and scraping must be performed for KOH preparation for demonstration of fungal elements.
Treatment:
- General measures: Keeping area dry; Avoiding use of synthetic clothes
- Antifungals:
- Topical:
- Terbinafine (Terfin) 1% cream BD X 2-4 weeks
- Ketoconazole (Ketoriv) Shampoo
- Systemic (For nail, scalp or extensive infections): For both itraconazole and griseofulvin, food increases
absorption.- Itraconazole 100 mg BD (Avoid in children and lactation) X 2-4 weeks
- Terbinafine 250 mg OD (5 mg/kg) X 4 weeks
- Finger nails: 6 weeks
- Kerion: 8 weeks
- Toe nails: 12 weeks
- Tine capitis: Griseofulvin 10-20 mg/kg/day. The tablets can be crushed and given with ice cream. Treatment should continue for 2–4 months, or for at least 2 weeks after negative laboratory examinations are obtained.
- Topical:
Classification of Antifungals:
- Imidazoles: clotrimazole, miconazole, econazole, sulconazole, oxiconazole, voriconazole, and ketoconazole.
- Inhibition of the cytochrome P450 14-α-demethylase, an essential enzyme in ergosterol synthesis.
- Polyenes: Nystatin
- Irreversibly binds to ergosterol, an essential component of fungal cell membranes.
- Allylamines: Naftifine, terbinafine, and butenafine
- Inhibition of squalene epoxydation.
- Pregnancy and lactation are relative contraindications. Theren have been reports of headaches, taste disturbances and, very rarely, liver dysfunction.
- Triazoles: Itraconazole and fluconazole
- Affect the cytochrome P450 system
- Cases of liver damage have rarely been reported.
- Benzofurans: Griseofulvin
- Binds to tubulin, interfering with microtubule function, thus inhibiting mitosis
- Contraindications to griseofulvin are severe liver disease and porphyrias.
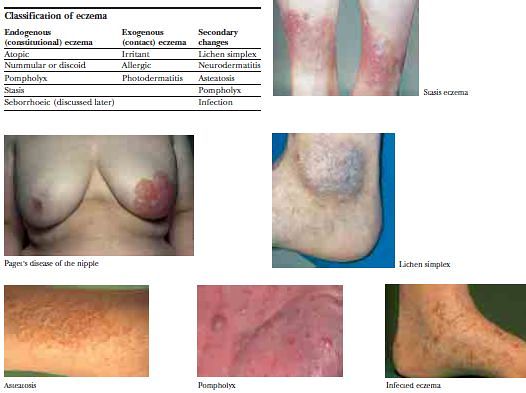
C) ECZEMA
Morphology:
- Acute Eczema:
- weeping and crusting
- blistering usually with vesicles
- redness, papules and swelling usually with an ill defined border
- scaling
- Chronic Eczema:
- less vesicular and exudative
- more scaly, pigmented and thickened
- more likely to show lichenification
- more likely to fissure.
Asymmetrical distribution, known contact history and temporal improvement on change of environment and removal of triggers suggest Exogenous eczema.
Triggers for endogenous eczema include stress, dryness, etc.
Symptoms: Pruritus and pain
Types:
- Atopic eczema: affects mainly the flexor surfaces of the elbows and knees as well as the face and neck; often have family history; usually children
- infant (onset at 2-6 months old): face, scalp, extensor surfaces
- childhood (>18 months): flexural surfaces
- adult: hands, feet, flexures, wrists, face, forehead, eyelids, neck
- Seborrheic eczema: greasy, erythematous, yellow, scaling papules and plaques in areas rich in sebaceous glands
- infants: one cause of cradle cap
- children: may be generalized with flexural and scalp involvement
- adults: diffuse involvement of scalp margin with yellow to white flakes, pruritus, and underlying erythema
- sites: scalp, eyebrows, eyelashes, beard, glabella, post-auricular, over sternum, trunk, body folds, genitalia
- Nummular eczema: appears as coin shaped lesions on legs and trunk
- Stasis eczema: around the ankles
- Lichen simplex: Localised area of lichenification produced by rubbing. Neurodermatitis is a term often used synonymously with lichen simplex.
- Asteatotic eczema: older people with a dry, “crazypaving” pattern, particularly on the legs
- Pompholyx: itching vesicles on the fingers, with lesions on the palms and soles in some patients
- Irritant contact dermatitis: Palmar surface of hand usually involved
- Allergic contact dermatitis: Dorsum of hand usually involved; often discrete area of skin involvement
- Chromate—in cement and leather
- Biocides, for example, formaldehyde and isothiazolinones, used in cutting oils in engineering
- Epoxy resins (uncured monomers)
- Rubber chemicals
- Hair dressing chemicals—particularly dyes and setting lotions
- Plant allergens
Infection can modify the presentation of any type of eczema or contact dermatitis.
Investigations:
- Allergic contact dermatitis: Patch test
- Photoallergic contact dermatitis: Photopatch test
- Atopic dermatitis: Prick test, serum IgE, RAST for IgE antibodies
Treatment:
a. Remove trigger
b. Wet, inflamed, exuding lesions:
- Use wet soaks with plain water, normal saline, or aluminium acetate (0·6%). Potassium permanganate (0·1%) solution should be used if there is any sign of infection.
- Use wet compresses rather than dry dressings (“wet wraps”).
- Steroid creams should be used.
- A combined steroid–antibiotic cream is often needed as infection readily develops.
- Systemic antibiotics may be required in severe cases. Take swabs for bacteriological examination first.
- Dry, scaling, lichenified lesions
c. Dry, scaling, lichenified lesions:
- Use emollients.
- Use steroid ointments, with antibiotics if infection is present.
- A weak coal tar preparation or ichthammol can be used on top of the ointments. This is particularly useful at night to prevent itching. 1–2% coal tar can be prescribed in an ointment. For hard, lichenified skin salicylic acid can be incorporated.
Topical steroids:
- Avoid long term use of strong steroids.
- Potent or very potent steroids should be applied sparingly and often for a short time, then a less potent preparation less
often as the condition improves. - Use only mildly potent steroids (that is, hydrocortisone) on the face.
- Use preparations combined with antibiotics or antifungals for the flexures.
Some commonly used steroids:
- Fusimar-h (Fusidic acid + Hydrocortisone): On face
- Metasone (Mometasone): On limbs
- Betameth -g or -s (Betamethasone + Gentamycin or Salycyclic acid): Most sites
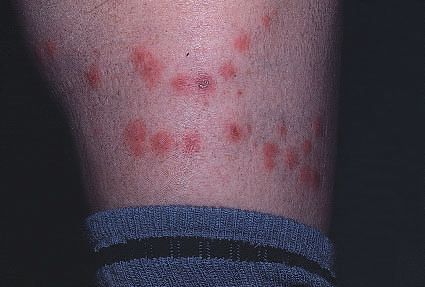
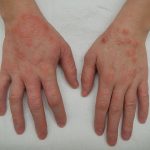
D) PAPULAR URTICARIA
Cause: Allergic reaction to bites of arthropods such as flea and mosquitoes
Presentation:
- Sites: arms or legs.
- Morphology: Groups or lines of small itchy excoriated smooth urticarial papules of a uniform size that may become bullous and infected. Some clear to leave small scars or pigmented areas.
- Symptoms: Pruritus
Course:
- Individual lesions last for 1 or 2 weeks and recur in distinct crops, especially in the summer
- The lesions will disappear with any change of environment, for example by going on holiday
Treatment:
- Prevention of repeated insect bites – protective clothings, insect repellents (eg. odomos)
- Topical steroids + Topical antibiotics
- Antihistaminics for pruritus
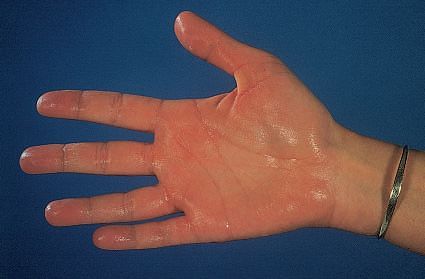
E) LOCAL HYPERHIDROSIS
Symptoms: Excessive sweating with or without foul odor
Sites: Palms, soles and axillae.
Consider: thyrotoxicosis, acromegaly, tuberculosis and Hodgkin’s disease, anxiety state
Precipitated by emotional stimuli and stops during sleep.
Treatment
- 20% aluminium chloride (Aldry)
- Potassium permanganate soaks (1 : 10 000 aqueous solution) combat the bacterial superinfection
- Glutaraldehyde solutions
- Iontophoresis. This is the passage of a low-voltage direct current across the skin. Iontophoresis with tap water or with the anticholinergic drug glycopyrronium bromide (glycopyrolate) may help palmar or plantar hyperhidrosis.
- Botox
- Surgery: Removal of sweat glands or symphatectomy

He is the section editor of Orthopedics in Epomedicine. He searches for and share simpler ways to make complicated medical topics simple. He also loves writing poetry, listening and playing music.